Why Thoracolumbar Implant Systems Are Essential for Spinal Surgery?
The significance of thoracolumbar implant systems in spinal surgery cannot be overstated. Dr. John Smith, an expert in spinal surgery, states, "Thoracolumbar implant systems are crucial for achieving spinal stability." This underscores their vital role in modern surgical procedures.
These systems provide essential support during recovery. They stabilize the spine, allowing for proper healing. Surgeons use them to correct deformities and address traumatic injuries. Each implant is designed with precision to ensure the best fit and functionality. However, the complexity of these systems requires continual innovation and expert handling.
Not all surgeries yield perfect results. Some complications can arise post-operation. It's crucial for surgical teams to remain vigilant. Evaluating the performance of thoracolumbar implant systems is essential for future improvement. Overall, these implants represent a blend of technology and expertise in spinal surgery, demanding ongoing reflection and refinement.
Understanding Thoracolumbar Implant Systems in Spinal Surgery
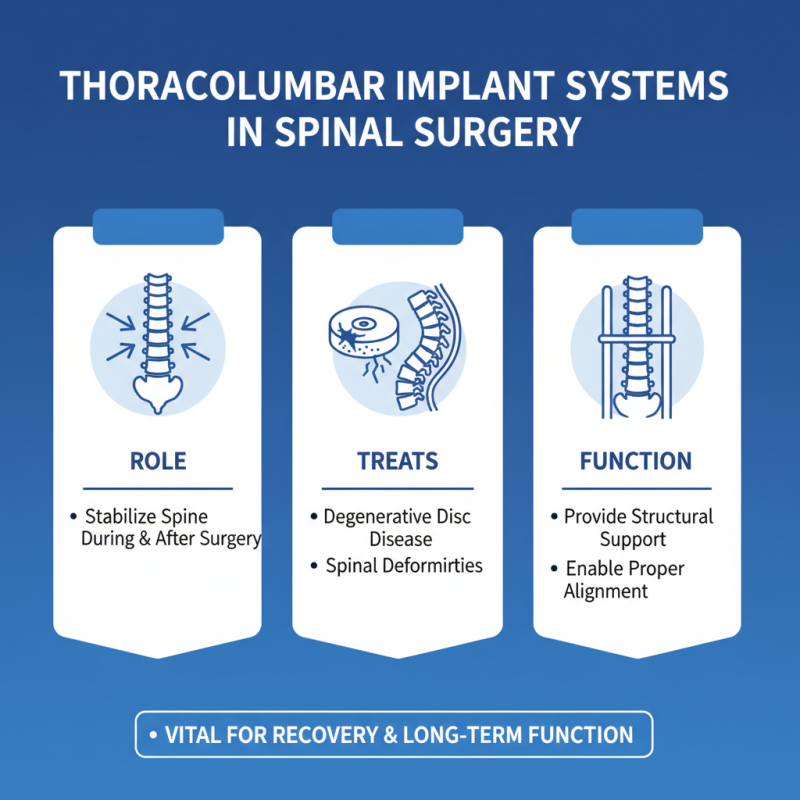
Thoracolumbar implant systems play a crucial role in spinal surgery. These systems stabilize the spine during and after corrective procedures. They are designed to treat various pathologies, including degenerative disc disease and spinal deformities. The implants provide structural support, enabling proper alignment of the vertebral column. This support is vital for patient recovery and long-term function.
Understanding how these systems work is essential for both surgeons and patients. Surgeons rely on their expertise to select the right implants based on individual needs. Each system is biomechanically engineered for specific levels of the spine. However, despite advancements, challenges remain. Complications may arise during surgery, such as misalignment or infection. Awareness of these risks is crucial for informed decision-making.
The reliability of thoracolumbar systems often comes down to surgical technique and patient factors. Not every implant suits all patients, and some may experience varying outcomes. Continuous research is needed to improve these systems. Surgeons must stay updated on innovations and refine their techniques. This reflects an ongoing commitment to enhance the efficacy and safety of spinal surgery overall.
The Anatomy of the Thoracolumbar Spine and Its Surgical Challenges
The thoracolumbar spine, comprising the lower thoracic and upper lumbar regions, presents unique surgical challenges. This region supports significant body weight and enables critical motion. It is essential to consider the anatomy, including vertebrae, discs, and surrounding soft tissues. Surgeons must navigate complex nerve pathways and vascular structures during procedures, which increases the risks involved.
Surgical interventions in this area often involve addressing issues like fractures, degeneration, and scoliosis. These conditions can create instability, leading to pain and disability. The challenges arise from the spine's intricate structure. A slight deviation during surgery can lead to severe complications. Moreover, the healing process can be unpredictable, forcing surgeons to be adaptable.
Thoracolumbar implant systems offer support and stability. These devices enhance the spine's structural integrity post-surgery. They can help surgeons achieve better alignment and promote healing. However, the choice of implant must be tailored to each patient’s specific anatomy and condition. The ongoing evolution of surgical techniques requires constant learning and adjustment in practice to improve outcomes.
Importance of Thoracolumbar Implant Systems in Spinal Surgery
This chart illustrates the impact assessment of various benefits associated with thoracolumbar implant systems in spinal surgery, highlighting their significance in enhancing stability, reducing recovery time, and improving patient outcomes.
Benefits of Using Implant Systems in Thoracolumbar Procedures
Thoracolumbar implant systems offer significant benefits for patients undergoing spinal surgery. These systems provide enhanced stability to the spine during recovery. They are designed to support vertebrae effectively, promoting proper alignment and fusion. Surgeons can achieve better outcomes, thanks to the precision offered by these implants.
Using implant systems helps reduce the risk of complications. They minimize movement at the surgical site, allowing for optimal healing. Patients often experience less postoperative pain and can return to their activities more quickly. The use of advanced materials ensures durability, yet there are still challenges in the selection process.
The decision to use specific implants requires careful consideration. Each patient’s anatomy and condition vary, necessitating personalized approaches. Additionally, while technology has improved significantly, not all systems guarantee the same results. Continuous evaluation and adaptation are vital in spinal surgery to ensure long-term success.
Types of Thoracolumbar Implant Systems and Their Applications
Thoracolumbar implant systems play a crucial role in spinal surgery. They stabilize the spine and facilitate healing. Different types of these systems serve varied applications in surgical procedures.
Common implants include rods, screws, and cages. Pedicle screws are especially favored for their strong fixation. A study published in the “Journal of Spinal Disorders” shows a 90% success rate for surgeries using these screws. Anterior cervical plates are effective for anterior approaches, promoting fusion in lower spine cases. Different designs cater to the unique needs of patients.
Integrating these systems greatly aids recovery. However, not every patient is a candidate. Comorbidities may limit options. Surgeons must weigh the risks carefully.
Future Trends in Thoracolumbar Implant Technologies and Techniques

The future of thoracolumbar implant technologies is promising. Innovations are emerging in materials, design, and techniques. These advancements aim to improve patient outcomes and enhance surgical efficiency. Bioactive materials are gaining interest. They help in bone integration and healing. Enhanced imaging technologies are also paving the way for precise implant placement. This minimizes complications during surgery.
Surgeons are experimenting with minimally invasive techniques. These approaches reduce recovery time and infection risk. However, challenges remain in training and mastering these skills. Not all surgeons have equal access to the latest technologies. The gap in knowledge and resources requires attention. Continuous education and hands-on experience are key for proficiency.
Additionally, there is a growing emphasis on personalized medicine. Tailoring implant systems to individual anatomical needs is crucial. Yet, this personalization must balance cost-effectiveness. The industry needs to reflect on how to make these advanced technologies accessible to all patients. There’s much to learn as we move forward in this dynamic field.